The International Association for the Study of Pain defines it as an “unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage.” This is obviously vague and completely insufficient, especially considering the tremendous variations of pain that can be experienced.
And indeed, a fundamental problem with measuring pain is that everyone feels it differently. Some people have a particularly high tolerance for it, while others are profoundly affected by the most unassuming of things. What’s needed, therefore, is a scale that takes this internal subjectivity and individual variation into account. 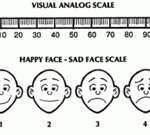
But frustratingly, there is no unified or industry-standard pain scale that has been accepted. There are over 20 different scales that are utilized in different jurisdictions and contexts. The lack of consensus on this issue points to how difficult it is to measure what is essentially phenomenological quale (the individualized or subjective experience of pain).
One standard pain scale is the Visual Analog Scale (VAS). By using illustrations, patients are asked to indicate the picture that most closely corresponds to how they are feeling. Advantages of this scale include its suitability for all age groups, and it doesn’t require the understanding of verbal or written descriptions. And in fact, studies show that, when implemented correctly, the scale can be useful.
Another popular scale that has been used widely in primary care settings is the Numeric Rating Scale (NRS). Healthcare workers using this scale ask their patients to rate their pain from 1 to ten, with ten being the most excruciating pain they can possibly imagine. Unfortunately, follow-up studies have shown that the NRS is only moderately accurate.
Part of the problem with the NRS is that different people can imagine different extremes of pain. Some patients understate their degree of physical discomfort when thinking about just how excruciating things can really get. And those with little experience with pain (or with poor imaginations) may overstate their degree of pain.
Similarly, people have a hard time quantifying the complexities and nuances of pain in something as simple as a scale from one to 10. Women who go through childbirth, for example, often hit a point where they turn inward and feel that time has essentially stopped as they brace themselves for the next contraction. How could something like this possibly be expressed in a scale — especially when it’s virtually impossible to re-imagine it after the fact? Moreover, pain that’s inflicted through childbirth will be qualitatively different in nature from pain that’s inflicted through, say, third-degree burns.
Consequently, the development of a more reliable, detailed, and descriptive scale would seem to be in order. But given the highly complex and subjective nature of pain, this may never happen. Non-Surgical Orthopaedics, P.C. specializes in Pain Management and routinely uses a variety of pain measurements and pain scales. Visit us at www.lowbackpain.com or call 770-421-1420.
